Clinical documentation has always been essential to good care, but it has never been the reason clinicians chose medicine.
SOAP notes, case notes, medical referral documentation, care plan samples are important parts of modern healthcare. They ensure continuity of care, support communication between providers, and protect both patients and clinicians. Yet for decades, the burden of producing them has quietly grown, expanding far beyond the time available in a standard consult.
AI scribe tools are often positioned as a simple solution: “dictate and your notes are done.” But that framing undersells both the problem — and the opportunity.
The real value of AI in healthcare documentation is not transcription alone.
From transcription to clinical workflow support
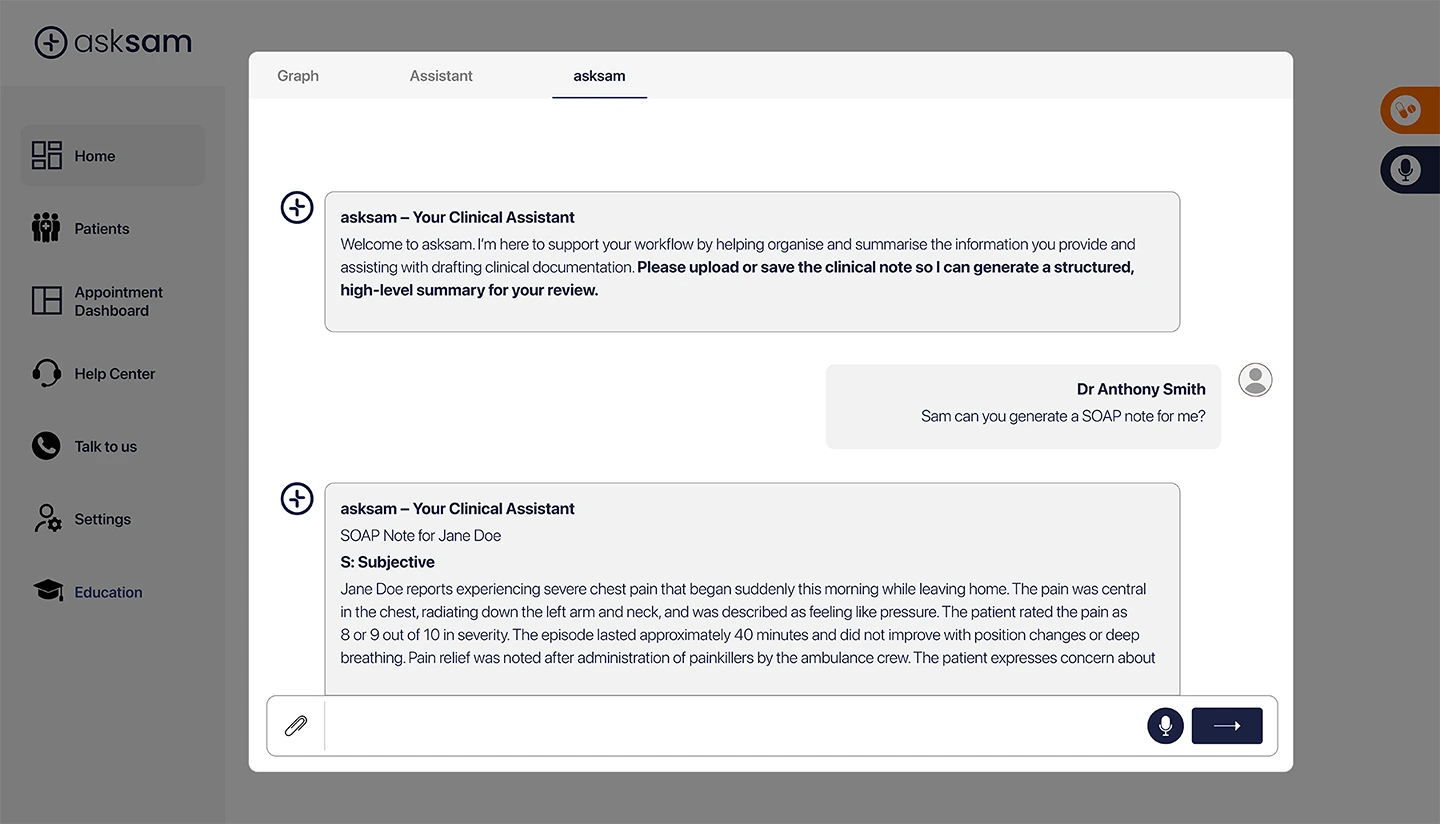
Traditional AI medical scribing tools focus on converting speech into text. They generate documents such as SOAP notes, save it, and stop there. While that alone can reduce typing time, it does little to address the downstream work that follows every consult.
A clinician doesn’t just need a SOAP note. They need case notes that fit into a longitudinal patient record. They should have medical referral documentation that reflects history, investigations, and intent, as well as care plans that are consistent with previous decisions, patient context, and current goals.
This is where the next generation of AI medical scribe tools matters.
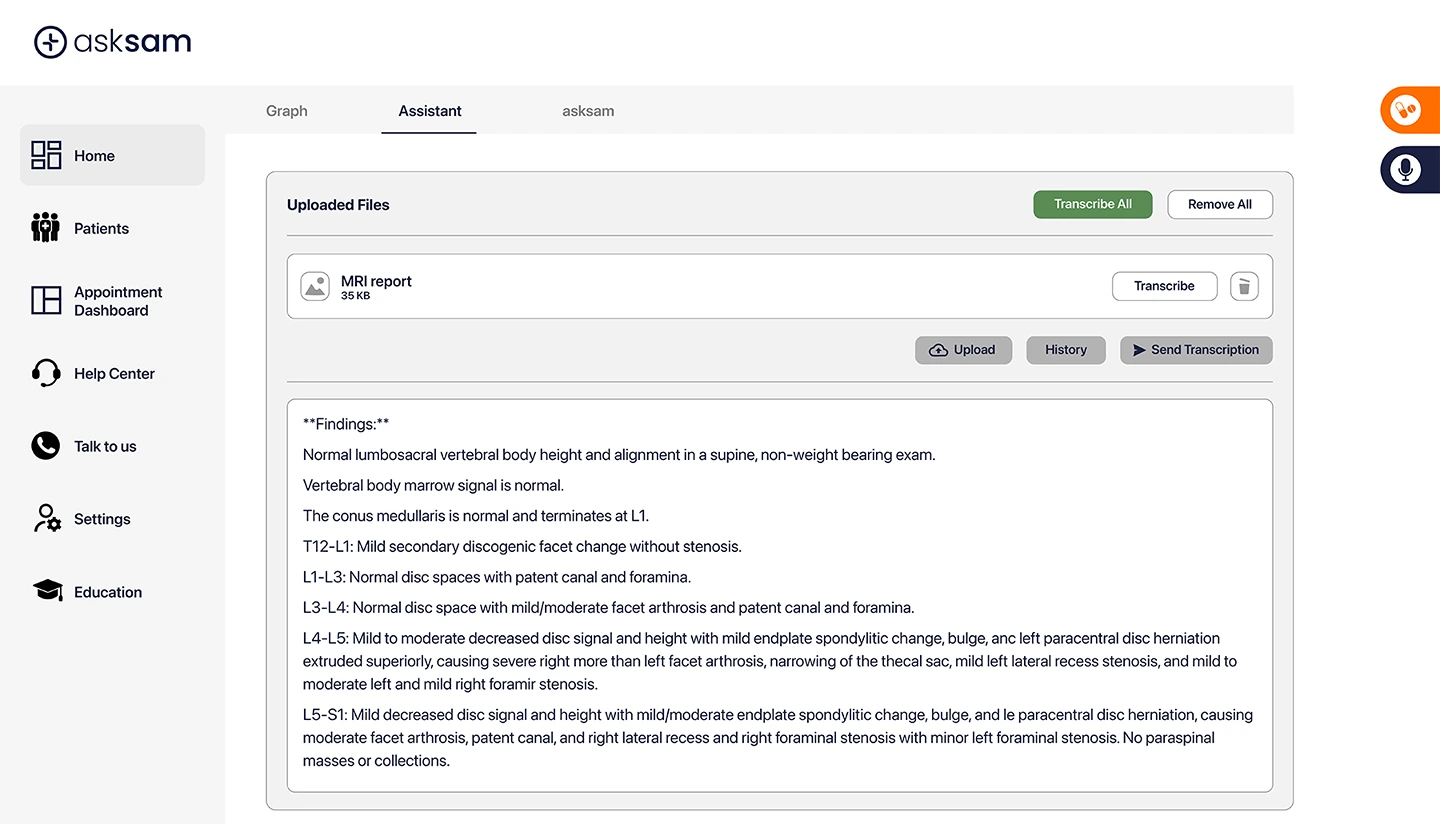
When AI understands clinical structure — rather than simply words — documentation becomes cumulative rather than repetitive. Notes connect to case files. Referrals draw from existing history. Care plans build on what’s already known instead of starting from scratch.
The result is not just faster documentation, but fewer gaps, fewer rewrites, and less mental load.
Consistency is an efficiency multiplier
One of the most underestimated challenges in clinical admin is inconsistency when generating SOAP notes, case notes and referrals.
AI scribing tools that support flexible but structured outputs help standardise documentation without forcing rigid templates. Clinicians can generate documents in their preferred format, while ensuring essential clinical elements are consistently captured. Medical referral documentation is clear, complete, and fit for purpose.
That consistency saves time well beyond the consult itself — when reviewing files, responding to queries, or continuing care across teams.
Documentation should reflect the whole patient, not just the last visit
Healthcare does not happen in isolated encounters, yet documentation often does.
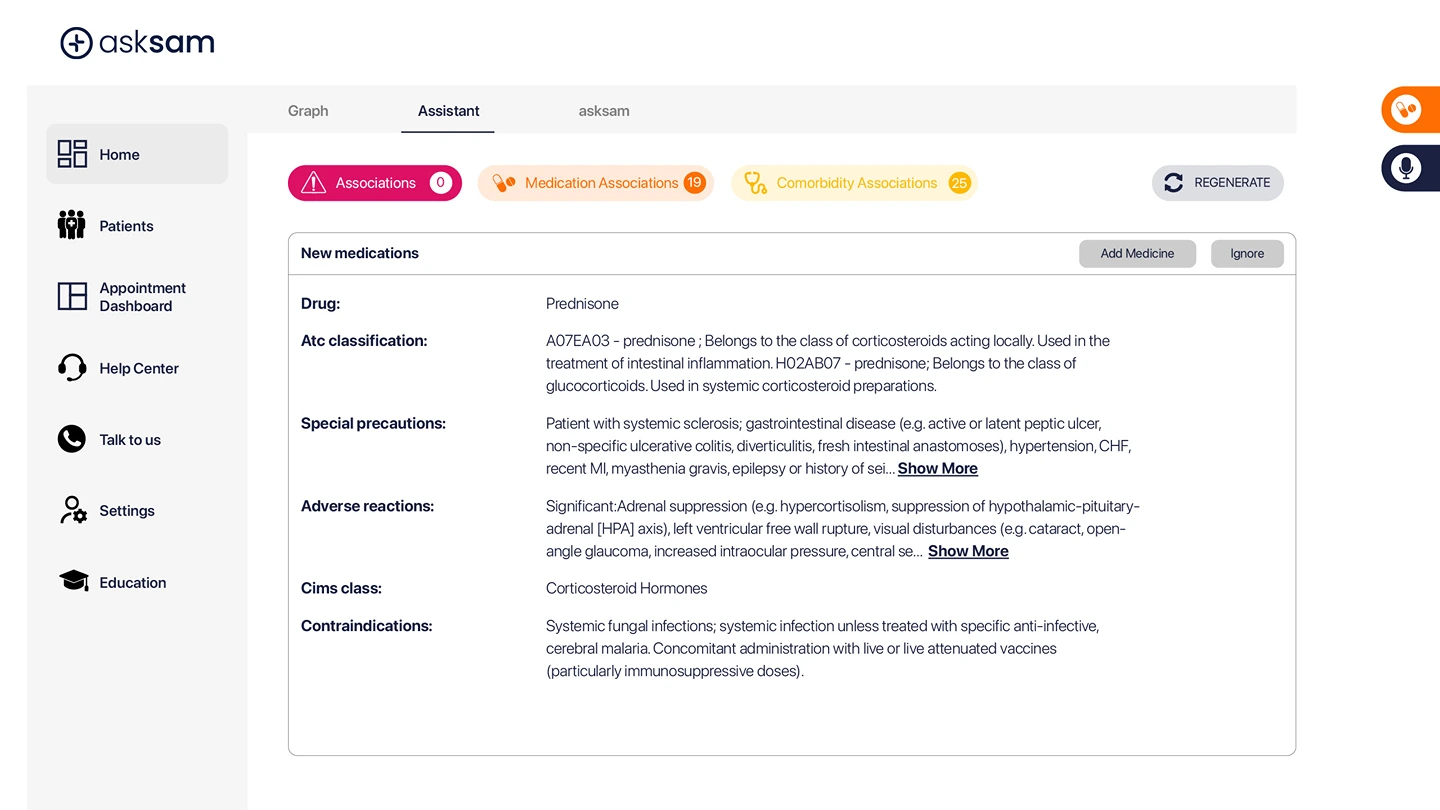
A common frustration for clinicians is rewriting the same background repeatedly: past history, medications, social context. AI scribing tools that integrate documentation into a holistic case file allow information to persist and evolve rather than being recreated.
This is particularly powerful for care plan samples. Instead of drafting plans in isolation, clinicians can generate care plans that reflect the patient’s documented journey — aligning goals, treatments, and follow-up in a way that feels coherent rather than administrative.
Efficiency, in this sense, is not about speed alone. It’s about reducing duplication and preserving clinical intent.
The role of trust in AI-generated documentation
Efficiency only matters if clinicians trust the output.
Healthcare documentation requires accuracy and context. AI scribing tools must operate within clear guardrails, using verified medical sources and clinician-controlled workflows. The goal is to support documentation, not replace professional judgement.
When clinicians trust that AI-generated SOAP notes, case notes, and medical referral documentation are accurate and remain fully editable, adoption follows naturally.
A shift worth getting right
AI scribing tools are no longer a novelty. They are becoming part of everyday practice. The real question is not whether clinicians should use them, but how thoughtfully they are integrated into clinical workflows.
Used well, AI can reduce administrative friction — freeing clinicians to focus on the human side of care while maintaining high-quality documentation.
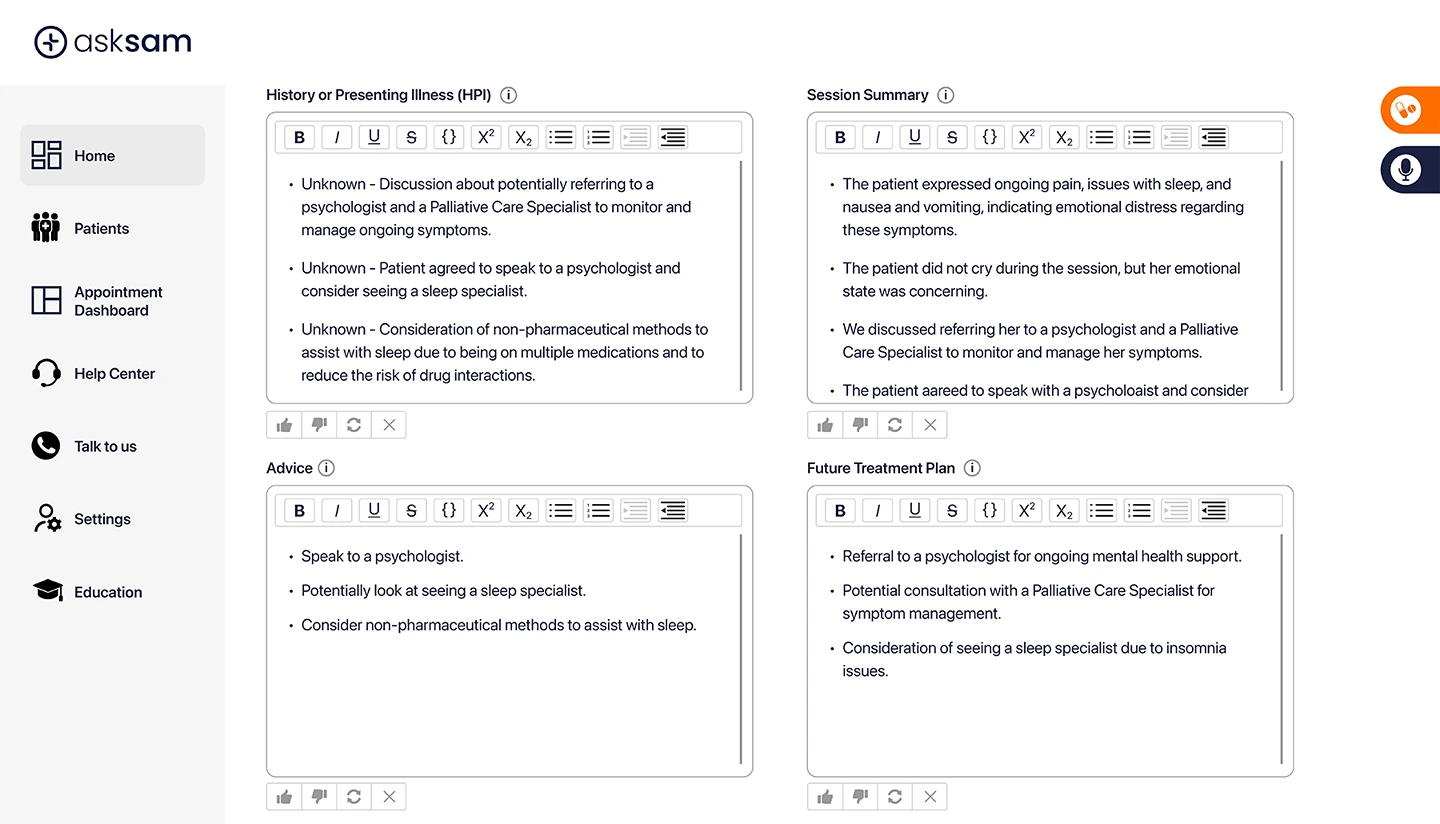
asksam™ was built with this philosophy in mind: more than a scribe, it’s your AI-powered clinical assistant — designed to support the full documentation lifecycle, not just the transcript.
Because efficiency in healthcare documentation isn’t about doing less work.
It’s about doing the right work properly and with confidence.